How can a Physiotherapist Assess and Treat Meniscus Tears in Knee Joint?
What is a Meniscus Tear?
The knee joint is formed by a total of four bones. The upper portion of the knee consists of the thigh bone, called the femur. The lower aspect is made of the two shin bones, called the tibia and the fibula. 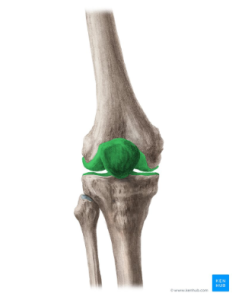 The tibia is the larger of the two and connects directly to the femur, providing knee flexion and extension. Whereas the smaller fibula bone articulates with the lateral aspect of the tibia and provides slight internal and external rotation movement and gliding movements to aid in dorsi and plantarflexion. Lastly, the fourth bone is called the patella, and the patella’s main role is to provide an insertion point for the quadriceps in order to increase lever lengths and generate more torque at the joint (force line is further from the rotational axis).
The tibia is the larger of the two and connects directly to the femur, providing knee flexion and extension. Whereas the smaller fibula bone articulates with the lateral aspect of the tibia and provides slight internal and external rotation movement and gliding movements to aid in dorsi and plantarflexion. Lastly, the fourth bone is called the patella, and the patella’s main role is to provide an insertion point for the quadriceps in order to increase lever lengths and generate more torque at the joint (force line is further from the rotational axis).
The knee is surrounded by connective tissues that form a capsule encompassing the knee joint. Included in these are the four collateral and cruciate ligaments connecting the femur to the tibia, as well as the series of multiple tendons, connecting the large muscle bodies, such as the hamstrings, quadriceps and gastrocnemius to the correlating bony insertion points. In addition to this, the menisci are two structures (medial and lateral) that sit within the joint space and act as shock absorbing, force distributing, friction reducing pads.
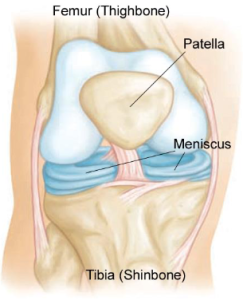 As with all soft tissues, when excessive forces are applied, the structure can fail and damages occur.
As with all soft tissues, when excessive forces are applied, the structure can fail and damages occur.
Who Gets Meniscus Tears?
Although meniscus tears can be both mechanical and degenerative, the group most at risk of obtaining a meniscal tear are those who participate in sports (0.51/10,000). In this instance, the meniscus is typically subject to compression, shear and rotation forces. However, meniscal tears can occur in older populations (40-60years), when age related degeneration begins to take place and activity levels are retained.
Other common risks factors for inversion sprains:
- Males
- Obesity
- Football and Rugby
- Work-related kneeling and squatting
How Common are Meniscus Tears?
Medial meniscus tears are a common musculoskeletal complaint.
Medial tears are 2-3 times more likely than lateral meniscus tears.
What are the Common Signs and Symptoms?
Common signs and symptoms include:
- Pain, especially when straightening, bending or twisting the knee.
- Severe, intermittent sharp pain may occur, and is localised to that side of the joint.
- Stiffness and loss of range may develop suddenly in the case of a traumatic event, or they may develop slowly, over the course of a few weeks.
- Swelling may occur soon after the injury or several hours later as a result of inflammation.
- You may experience a ‘locking’, ‘catching’ or ‘giving way’ sensation as the tear or flap may affect joint mechanics.
- Complaints of clicking, popping within the knee may also follow a meniscus injury.
Meniscal tears often occur in conjunction with other knee related injuries, the most common is damage to the anterior cruciate ligament (ACL). This may be due to the susceptibility of both structures to fail under the similar (axial, rotational and shearing) force profile.
Differential Diagnoses
Collateral/Cruciate Ligament Tears – damage to the collateral/cruciate ligamentdiscussed earlier
Knee OA – Arthritis affecting the knee joint.
Patellar Tendinopathy – Irritation at the tendon between the kneecap and shin bone.
ITB syndrome – Pain in the lateral knee, originating from the iliotibial band.
Assessments/Tests
What makes it worse?
- Symptoms may worsen with standing, walking and running
- Movements such as twisting, squatting, getting in and out of a car
- Rolling over in bed may increase pain and cause broken sleep
- Palpation (pressing) on the inner or outer joint line
- Symptoms can often worsen at night or first thing in the morning
What do people tell us? (Subjective)
- Stabbing Pain, often localised to the inside/outside of the knee joint line
- Knee locking with completing certain tasks
- Reduced movement or sensations such as clicking, popping, catching when moving
- Often there is minimal swelling
- Trouble sleeping especially on the affected side
What do we find on physical assessment/testing? (Objective)
Visual – The patient may display an altered gate to reduce pressure on the joint. Visual inflammation is often not apparent.
Palpation – There may be pain around the anterolateral/medial joint line, depending on the side of the affected meniscus.
Range of Motion – Meniscus tears can often affect the range of motion available at a joint. This may be down to a couple of reasons:
- The tear may cause a flap of cartilage that can cause the joint to become locked in a certain position. This will often resolve quickly.
- The tear may cause some movements to become painful such as total extension/flexion.
Strength – Strength may be affected in the limb. Altered gait and reduced usage may have resulted in muscle atrophy which will in turn reduce the strength/power available at the local and surrounding joints.
Diagnostic Clusters
There are two diagnostic clusters that are currently undergoing a trailing process in Canada by Décary, S et al. (2018). They look at the following two protocols and aim to accurately predict OA through the use of them alone.
| Diagnostic Cluster 1 50-58yrs AND BMI ≥30kg/m2 AND Varus or valgus knee misalignment OR Limited passive knee extension ROM |
Diagnostic Cluster 2 >58yrs AND Crepitus on palpation of any compartments |
Special Tests
- McMurray’s test (lying in supine, passive lower limb movements from flexion and internal or external rotation to extension) sensitivity of 61% and a specificity of 84%.
- Joint line tenderness (palpating around the anterolateral and anteromedial joint line) sensitivity of 83% and a specificity of 83%.
- Thessaly 20° (in single leg standing, perform internal/external rotation around a knee at 20° of flexion) sensitivity of 75% and a specificity of 87%.
Investigations/Scans
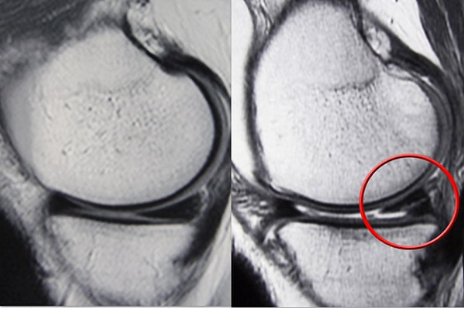
Magnetic Resonance Imaging (MRI)
An MRI scan assesses the soft tissues in your knee joint, including the menisci, cartilage, tendons, and ligaments. Magnetic Resonance Imaging is the most extensive imaging assessment of the knee and it is also cost effective and can aid in prognosis and further treatment options when it is performed early after injury.
CT- scan – Computed tomography is generally reserved for diagnosis of suspected fractures or assessment of complex fractures, although associated ligamentous injuries can be observable on CT scans intended for evaluation of osseous injuries.
X-Ray – X-rays provide images of dense structures, such as bone. Although an X-ray will not show a meniscus tear, your doctor may order one to look for other causes of knee pain, such as osteoarthritis.
Treatments
Conservative Treatment
Physiotherapy
For simple tears confined to the outer 1/3 of the meniscus and degenerative tears, it is reasonable to perform a 4-6 week course of relative rest and physical therapy to determine if spontaneous healing and return to the desired level of function will occur.
| Passive Rehab | Active Rehab |
| PEACE Protocols Protect – Protect from further injury Elevate – avoid pooling Avoid NSAIDS – allow inflam. cycle Compress – reduction of inter Education – avoid catatrophising/fear | LOVE Protocols Load Optimally – load that structure! Optimism – Be positive, it will heal. Vascularisation – early mobilisation and increased Exercise – get back into pain free movement! |
| Manual therapy – Mobilsation and manipulation movements can be used to aid in pain relief and range of motion in the short term. | Mobility training – There is debate surrounding the use of stretching in the reactive stages of tendinopathies. This is due to the compressive nature that can come alongside stretches. As a general rule, stretches should be participated in a position to mitigate pain response. |
| Acupuncture – Localised microtrauma, increases blood flow to the local area. Pain experience modulation Neurotags | Strength training – Strength training should be focussed on the biceps, rotator cuff and scapula stabiliser muscle groups. |
Some additional treatments that a physio may offer you:
- Taping for support and pain relief
- Advice on supplements for pain reduction and injury recovery
- Possible gait assessment
- Specialist equipment, such as orthotics, bracing, and rehabilitation equipment
Home exercises that may help – V = check out our YouTube for example videos!
Stretching
- Active knee straightening (push down into floor/towel)
- Supine heel slides (using a band)
- Single leg standing hamstring stretch
- Knee ext. With rolled towel on heel
- Kneeling rock backs.
Strengthening
- Straight/bent leg, single leg stands
- Banded knee extensions
- Bridging
- Bridging with sliders
- Side planks/Copenhagen plank
Exercises you may progress towards as you become stronger:
- Balance – reaching out of BOS, Y foot taps
- strength –
- plyometrics – single leg hops, skips,
Pilates specific:
Trapezius: Thigh stretch,
Multi chair: Step ups, leg work double?
Reformer: Scooter, Russian splits, Side adb/add/squat.
Non-conservative Treatment
Despite conservative management, patients with persistent pain, swelling, and mechanical symptoms should be assessed for potential non-conservative intervention. The outer third of the meniscus has a good blood supply (the “red zone”), but the inner two thirds has no blood supply. This means that injuries to the inner parts of the meniscus have a low capacity to heal.
Corticosteroid Injections
Steroidal injections have been found to provide an positive anti-inflammatory response, and are a beneficial tool when used to target acute-stage over exertion of the tissues. However, overuse or repetitive strain injuries injuries treated with solely anti-inflammatory agents such as this will only see benefits short term, with a high likelihood of symptoms resurfacing over the future weeks/months when activity is continued. Injections tend to produce short-lasting results, with profound effects lasting an average of up to 4 weeks.
Surgery
Initial treatment of meniscal tears is conservative care, protect, elevate, ice, compression and education regarding the injury. This is usually combined with analgesia such as a non- steroidal anti-inflammatory medication.
Some tears, particularly those near the outer rim, can heal naturally.
The outer third of the meniscus (the “red zone”) has a good blood supply, but the inner two thirds has no blood supply. This means that injuries to the inner parts of the meniscus have a low capacity to heal.
Patients with injuries that occur more centrally, or experience ongoing meniscal symptoms, may be treated with surgery. These options are dependent on the type of tear.
Bucket handle tears of the meniscus which run parallel to the edge of the meniscus are the most readily repairable. When the tear is irreparable, the margins of the tear can be resected to eliminate any unstable flaps causing pain.
A few factors influencing whether the meniscus should be repaired include:
- Patient age – younger patients are more likely to benefit from meniscal repair.
- Location of the tear – loss of the lateral meniscus is associated with poorer outcomes than loss of the medial meniscus.
- Type of tear – bucket handle tears are the most amenable to repair. Degenerate and horizontal tears are usually best removed.
- Presence of arthritis – once degenerative change in the joint occurs, there may be limited benefit from repairing the meniscus.
Knee arthroscopic surgery is one of the most common procedures performed annually. Knee arthroscopy is generally considered the gold standard in diagnosis and simultaneous treatment of meniscus disorders.
With an arthroscopy, the surgeon inserts a small device called an arthroscope into the incision. The surgeon uses the arthroscope to look at the tear and decide what surgical technique to perform:
- Meniscus repair: Using a suture, the surgeon sews any torn pieces of cartilage together to aid in the healing process. The outcome of this is largely dependent on the area of the tear.
- Partial meniscectomy: The surgeon trims and removes the damaged cartilage and leaves healthy meniscus tissue in place.
Recovery times following knee arthroscopy are generally 3-6 months.
Prehab
Prehab prior to surgery should look to increase the strength, range and stability of the knee joint, and prepare the patient for post-operative exercise regimes.
For instance the initial exercise program may include:
- Isometric Hamstring Contraction
- Isometric Quadriceps Contraction
- Sitting Straight Leg Raises
- Sitting Buttock Tucks
- Standing Straight Leg Raises
Generally, post operative exercise management is guided by the multidisciplinary team consisting of the orthopaedic surgeon and the physiotherapist.
Here is an example of a generic plan. However, depending on the surgery, the surgeon, the physiotherapist and the patient, the rehab may diffe
Initial Exercise Program | Intermediate Program | Advanced Program |
| Hamstring Contraction Quadriceps Contraction Straight Leg Raises Buttock Tucks Straight Leg Raises, Standing | Terminal Knee Extension, Supine Straight Leg Raises Partial Squat, with Chair Quadriceps Stretch, Standing | Knee Bend, Partial/Single Leg Step-ups, Forward Step-ups, Lateral Terminal Knee Extension, Sitting Hamstring Stretch, Supine Hamstring Stretch, Supine at Wall |
Décary, S, Feldman, D, Frémont, P, et al. Initial derivation of diagnostic clusters combining history elements and physical examination tests for symptomatic knee osteoarthritis. Musculoskeletal Care. 2018; 16: 370– 379. https://doi.org/10.1002/msc.1245